
10:00am to 04:00pm (Mon to Sat) - Amrita Hospital, Faridabad
06:00pm to 08:00pm (Mon to Sat) - Arthrocare Clinic, Noida
10:00am to 04:00pm (Mon to Sat) - Amrita Hospital, Faridabad
06:00pm to 08:00pm (Mon to Sat) - Arthrocare Clinic, Noida
 June 1, 2021
June 1, 2021
What is total hip replacement?
Total hip replacement is a surgical procedure in which parts of an arthritic or damaged joint are removed and replaced with a metal, plastic or ceramic device called a prosthesis. The prosthesis is designed to replicate the movement of a normal, healthy joint. The damaged ball (the upper end of the femur) is replaced with a metal ball attached to a metal stem that is fitted into the femur, and a plastic socket is implanted into the pelvis, replacing the damaged socket.
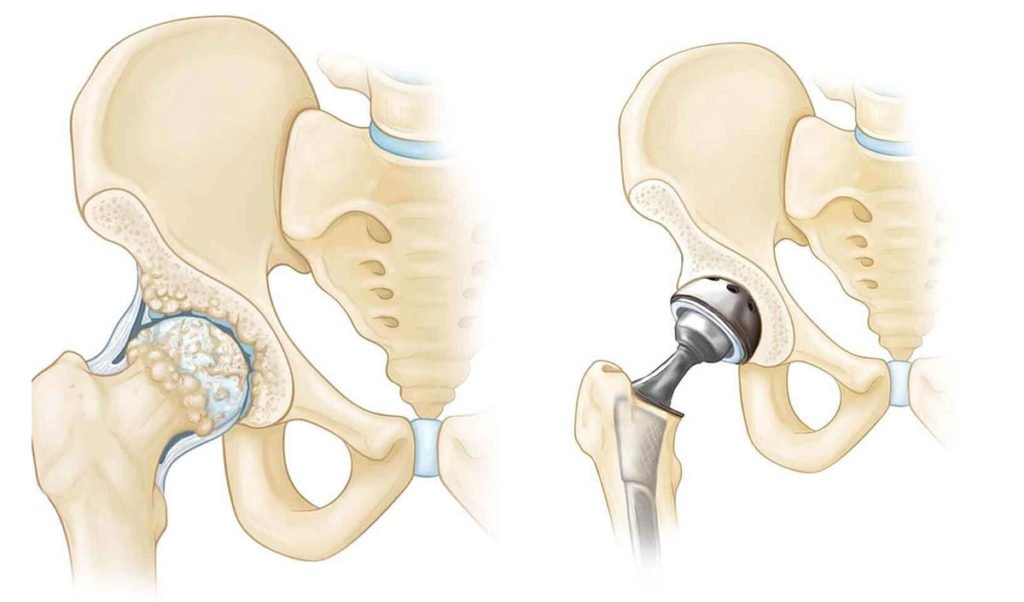
Do you require total hip replacement?
Common causes of chronic hip pain and disability are Osteoarthritis, rheumatoid arthritis, and traumatic arthritis that make everyday activities painful. Your hip may be damaged by arthritis, a fracture, or other conditions, common activities such as walking or getting in and out of a chair may be painful and difficult. Your hip may be stiff, and it may be hard to put on your shoes and socks. You may even feel uncomfortable while resting. Hip pain that continues while resting, Stiffness in a hip that limits the ability to move and pain is not relieved by anti-inflammatory drugs, physical therapy, or walking supports. You need a total hip replacement.
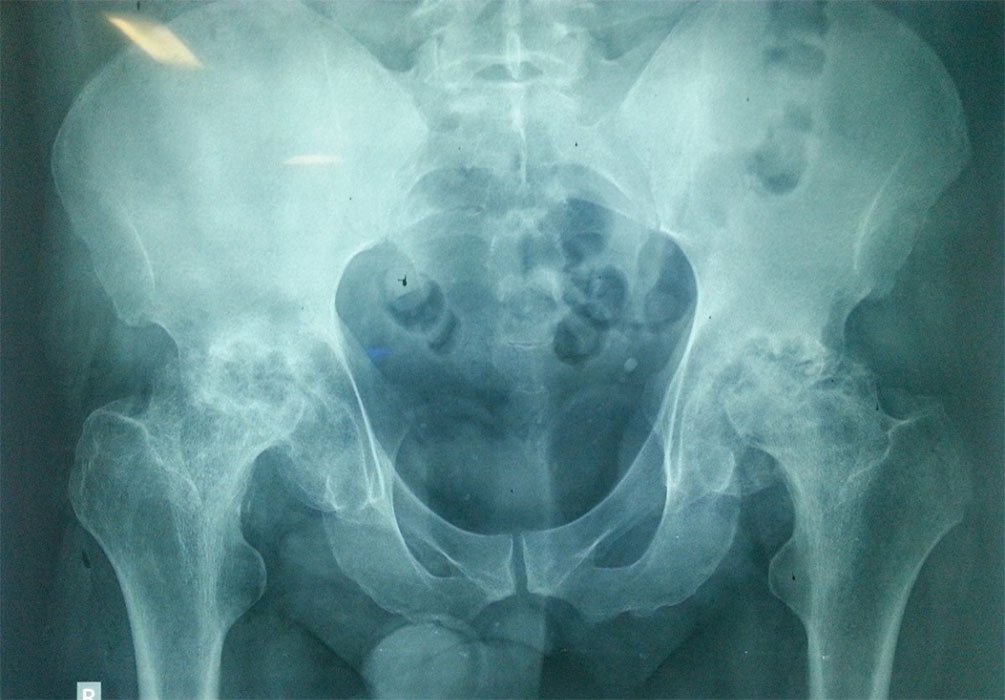
What components are used in total hip replacement?
The damaged ball of the hip joint is replaced with a ceramic or metal ball which fits on top of a titanium stem that fits into the femoral canal. The acetabulum is replaced with a metal shell with a highly cross-linked polyethylene or a ceramic liner.
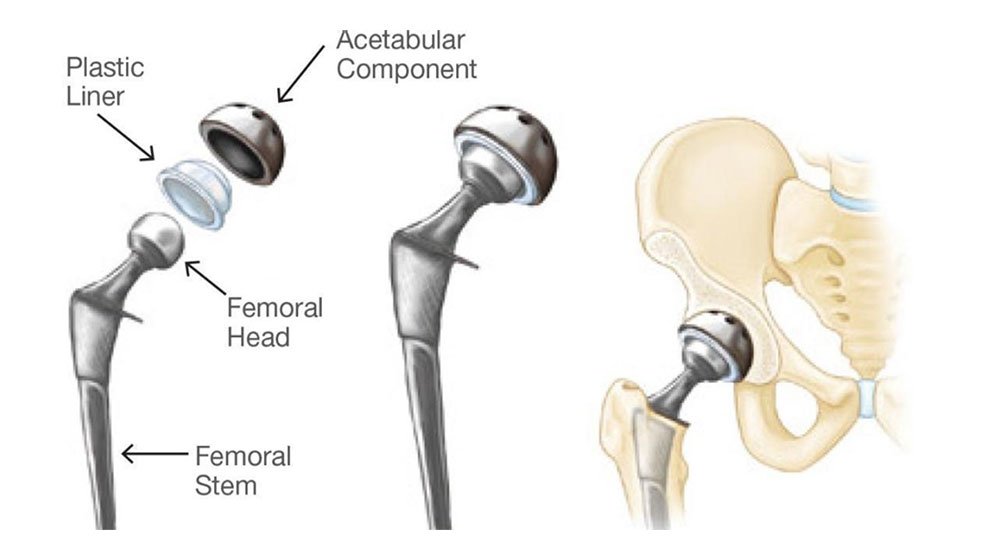
What is the pre-operative preparation?
Routine blood and urine tests are done before surgery followed by a pre anaesthetic checkup. You may be advised to donate your own blood prior to surgery. It will be stored in the event you need blood after surgery.
Tell your cancer surgeon about the medications you are taking. He or she or your primary care cardiologist will advise you which medications you should stop taking and which you can continue to take before surgery.
If you are overweight, your doctor may ask you to lose some weight before surgery to minimize the stress on your new hip and possibly decrease the risks of surgery.
Individuals with a history of recent or frequent urinary infections should have a urological evaluation before surgery. Older men with prostate disease should consider completing the required treatment before having surgery.
What complications can occur in or after surgery?
Some of the more common complications of joint replacement surgery include infection, blood clots, nerve injury, and prosthesis problems like loosening or dislocation.
What is the recovery process?
Patients are started in bed physiotherapy on the same day of surgery. Exercises such as ankle-toe movements, static quadriceps are taught. Check Xrays are done the next day. The patients are mobilised the next day. On the second day, they are taught toilet training mobilisation with a walker. Most patients will experience some temporary pain in the replaced joint because the surrounding muscles are weak from inactivity, the body is adjusting to the new joint, and the tissues are healing. This pain should resolve in a few weeks. Stitch removal is done in 2 weeks.
Exercise is an important part of the recovery process. Most people who undergo hip replacement surgery experience a dramatic reduction of hip pain and a significant improvement in their ability to perform the common activities of daily living.
What are the precautions after the Surgery?
How often do I need to see the doctor?
You have to be in a regular follow-up with your doctor. You would be visiting at 2 weeks, 6 weeks, 3 months, one year, three years and 5 yearly after surgery.



© 2024 Dr. Mrinal Sharma | All rights reserved. Designed and Developed by DigiTrend